Diabetes
Diabetes mellitus is a group of metabolic diseases characterized by high blood sugar (glucose) levels that result from defects in insulin secretion, or its action, or both. Diabetes mellitus, commonly referred to as diabetes was first identified as a disease associated with “sweet urine,” and excessive muscle loss in the ancient world. Elevated levels of blood glucose (hyperglycemia) lead to spillage of glucose into the urine, hence the term sweet urine.
What is the impact of diabetes?
Over time, diabetes can lead to blindness, kidney failure, and nerve damage. These types of damage are the result of damage to small vessels, referred to as microvascular disease. Diabetes is also an important factor in accelerating the hardening and narrowing of the arteries (atherosclerosis), leading to strokes, coronary heart disease, and other large blood vessel diseases. This is referred to as macrovascular disease.
Type 1 diabetes occurs when the body’s own immune system destroys the insulin-producing cells of the pancreas (called beta cells).
Normally, the body’s immune system fights off foreign invaders like viruses or bacteria. But for unknown reasons, in people with type 1 diabetes, the immune system attacks various cells in the body. This results in a complete deficiency of the insulin hormone.
Symptoms :
Symptoms of type 1 diabetes usually develop quickly, over a few days to weeks, and are caused by blood sugar levels rising above the normal range (hyperglycemia). Early symptoms may be overlooked, especially if the person has recently had an illness, such as influenza (flu). Early symptoms include:
 Frequent urination, which may be more noticeable at night. Some young children who have learned to use the toilet may start wetting the bed during naps or at night.
Frequent urination, which may be more noticeable at night. Some young children who have learned to use the toilet may start wetting the bed during naps or at night.
 Extreme thirst and a dry mouth.
Extreme thirst and a dry mouth.
 Weight loss.
Weight loss.
 Increased hunger (possibly).
Increased hunger (possibly).
Sometimes the blood sugar level rises excessively before a person knows something is wrong. Because insulin is not available, the cells in the body are unable to get the sugar (glucose) they need for energy. The body begins to break down fat and muscle for energy. When fat is used for energy, ketones-or fatty acids-are produced and enter the bloodstream, causing the chemical imbalance diabetic ketoacidosis. This is a life-threatening condition. Symptoms of diabetic ketoacidosis are:
 Flushed, hot, dry skin.
Flushed, hot, dry skin.
 Loss of appetite, abdominal pain, and vomiting.
Loss of appetite, abdominal pain, and vomiting.
 A strong, fruity breath odor.
A strong, fruity breath odor.
 Rapid, deep breathing.
Rapid, deep breathing.
 Restlessness, drowsiness, difficulty waking up, confusion, or coma. Young children may lack interest in their normal activities
Restlessness, drowsiness, difficulty waking up, confusion, or coma. Young children may lack interest in their normal activities
Cause :
Type 1 diabetes develops because the body’s immune system destroys the beta cells which are in the islet tissue in the pancreas.These beta cells produce insulin. So people with type 1 diabetes cannot make their own insulin.
Blood tests include:
 Hemoglobin A1c, a test that estimates your blood sugar over the past 2 to 3 months.
Hemoglobin A1c, a test that estimates your blood sugar over the past 2 to 3 months.
 Blood glucose test, a test that measures your blood sugar. This test is done preferably after fasting, but it can be done at any time, even if you have recently eaten.
Blood glucose test, a test that measures your blood sugar. This test is done preferably after fasting, but it can be done at any time, even if you have recently eaten.
Other tests that may suggest diabetes
You may need a thyroid-stimulating hormone (TSH) test when type 1 diabetes is diagnosed and then every 1 to 2 years
Treatment For Adults
Type 1 diabetes requires lifelong treatment to keep blood sugar levels within a target range. Treatment includes:
 Taking several insulin injections every day or using an insulin pump.
Taking several insulin injections every day or using an insulin pump.
 Monitoring blood sugar levels several times a day using a home blood sugar meter.
Monitoring blood sugar levels several times a day using a home blood sugar meter.
 Eating a healthful diet that spreads carbohydrate throughout the day, to prevent high blood sugar levels after meals.
Eating a healthful diet that spreads carbohydrate throughout the day, to prevent high blood sugar levels after meals.
 Regular physical activity or exercise, because exercise helps the body to use insulin more efficiently. Exercise may also lower your risk for heart and blood vessel disease.
Regular physical activity or exercise, because exercise helps the body to use insulin more efficiently. Exercise may also lower your risk for heart and blood vessel disease.
 Regular medical checkups to monitor and adjust treatment as needed. Screening tests and exams need to be done regularly to watch for signs of complications, such as eye, kidney, heart, blood
Regular medical checkups to monitor and adjust treatment as needed. Screening tests and exams need to be done regularly to watch for signs of complications, such as eye, kidney, heart, blood  vessel, and nerve diseases.
vessel, and nerve diseases.
 Not smoking.
Not smoking.
 Not drinking alcohol if the person is at risk for periods of low blood sugar.
Not drinking alcohol if the person is at risk for periods of low blood sugar.
A regular daily schedule makes managing blood sugar levels easier. Blood sugars are easier to predict and control when mealtimes, amounts of food, and exercise are similar every day.
Type 2 diabetes, once called non-insulin dependent diabetes, is the most common form of diabetes.
Unlike people with type 1 diabetes, people with type 2 diabetes produce insulin; however, either their pancreas does not produce enough insulin or the body cannot use the insulin adequately. This is called insulin resistance. When there isn’t enough insulin or the insulin is not used as it should be, glucose (sugar) can’t get into the body’s cells. When glucose builds up in the blood instead of going into cells, the body’s cells are not able to function properly.
Other problems associated with the buildup of glucose in the blood include:
 Damage to the body – Over time, the high glucose levels in the blood may damage the nerves and small blood vessels of the eyes, kidneys, and heart and predispose a person to atherosclerosis (hardening) of the large arteries that can cause heart attack and stroke.
Damage to the body – Over time, the high glucose levels in the blood may damage the nerves and small blood vessels of the eyes, kidneys, and heart and predispose a person to atherosclerosis (hardening) of the large arteries that can cause heart attack and stroke.
 Dehydration – The buildup of sugar in the blood can cause an increase in urination. When the kidneys lose the glucose through the urine, a large amount of water is also lost, causing dehydration.
Dehydration – The buildup of sugar in the blood can cause an increase in urination. When the kidneys lose the glucose through the urine, a large amount of water is also lost, causing dehydration.
 Diabetic Coma (Hyperosmolar nonketotic diabetic coma) – When a person with type 2 diabetes becomes very ill or severely dehydrated and is not able to drink enough fluids to make up for the fluid losses, they may develop this life-threatening complication.
Diabetic Coma (Hyperosmolar nonketotic diabetic coma) – When a person with type 2 diabetes becomes very ill or severely dehydrated and is not able to drink enough fluids to make up for the fluid losses, they may develop this life-threatening complication.
Type 2 Diabetes in Children
More and more children are being diagnosed with type 2 diabetes. Find out about type 2 diabetes symptoms in children, the diagnosis, and the treatment in WebMD’s article on type 2 diabetes in childhood. If your child is at risk for childhood diabetes, it’s important to learn specific self-care tips to help prevent diabetes.
Who Gets Type 2 Diabetes?
Anyone can get type 2 diabetes. However, those at highest risk for the disease are those who
 Are over 45
Are over 45
 Are obese or overweight
Are obese or overweight
 Have had gestational diabetes
Have had gestational diabetes
 Have family members who have type 2 diabetes
Have family members who have type 2 diabetes
 Have prediabetes
Have prediabetes
 Are inactive
Are inactive
 Have low HDL cholesterol or high triglycerides levels
Have low HDL cholesterol or high triglycerides levels
 Have high blood pressure
Have high blood pressure
 Are members of certain racial or ethnic groups
Are members of certain racial or ethnic groups
What Causes Type 2 Diabetes?
 When the pancreas does not produce any insulin.
When the pancreas does not produce any insulin.
 When the pancreas produces very little insulin.
When the pancreas produces very little insulin.
 When the body does not respond appropriately to insulin, a condition called “insulin resistance.”
When the body does not respond appropriately to insulin, a condition called “insulin resistance.”
Health Risk Factors for Type 2 Diabetes
 Type 2 diabetes is believed to have a strong genetic link, meaning that it tends to run in families.
Type 2 diabetes is believed to have a strong genetic link, meaning that it tends to run in families.
Other type 2 diabetes risk factors include the following:
 High blood pressure
High blood pressure
 High blood triglyceride (fat) levels
High blood triglyceride (fat) levels
 Gestational diabetes or giving birth to a baby weighing more than 9 pounds
Gestational diabetes or giving birth to a baby weighing more than 9 pounds
 High-fat and carbohydrate diet
High-fat and carbohydrate diet
 High alcohol intake
High alcohol intake
 Sedentary lifestyle
Sedentary lifestyle
 Obesity or being overweight
Obesity or being overweight
 Aging: Increasing age is a significant risk factor for type 2 diabetes. The risk of developing type 2 diabetes begins to rise significantly at about age 45 years, and rises considerably after age 65 years.
Aging: Increasing age is a significant risk factor for type 2 diabetes. The risk of developing type 2 diabetes begins to rise significantly at about age 45 years, and rises considerably after age 65 years.
What Is Diabetes Insipidus?
When most people hear “diabetes,” they think of diabetes mellitus. That’s a condition in which blood sugars are chronically elevated. In fact, diabetes is a general term for conditions that cause increased urine production. And when it comes to increased urine production, diabetes insipidus takes the cake. Diabetes insipidus is caused by problems related to a hormone called antidiuretic hormone or its receptor. Antidiuretic hormone (ADH) is produced in a part of the brain called the hypothalamus. It’s stored in the brain’s pituitary gland. Release of ADH causes the kidneys to hold onto water, which makes urine more concentrated.
symptoms of diabetes insipidus:
 Excessive thirst
Excessive thirst
 Excessive urine production (polyuria)
Excessive urine production (polyuria)
In some people, these symptoms can become extreme, causing dehydration.
Excessive fluid losses can also cause electrolyte imbalances. Possible symptoms include:
 Unexplained weakness
Unexplained weakness
 Lethargy
Lethargy
 Muscle pains
Muscle pains
 Irritability
Irritability
How Is Diabetes Insipidus Diagnosed?
 People with diabetes insipidus often seek medical attention because of their symptoms of excessive thirst and urination.
People with diabetes insipidus often seek medical attention because of their symptoms of excessive thirst and urination.
 Diagnosing diabetes insipidus requires serial measurements of blood and urine in a doctor’s office over several hours. The person goes without water during this time and gets progressively thirstier. The concentrations of sodium in the blood and urine are determined over time. An ADH substitute might then be administered to see if the person’s kidneys respond to it by concentrating the urine. The laboratory values and response to ADH can make the diagnosis.
Diagnosing diabetes insipidus requires serial measurements of blood and urine in a doctor’s office over several hours. The person goes without water during this time and gets progressively thirstier. The concentrations of sodium in the blood and urine are determined over time. An ADH substitute might then be administered to see if the person’s kidneys respond to it by concentrating the urine. The laboratory values and response to ADH can make the diagnosis.
How Is Diabetes Insipidus Treated?
 The most important part of treatment for diabetes insipidus is to drink plenty of fluids. That will replace the constant loss of water through the urine.
The most important part of treatment for diabetes insipidus is to drink plenty of fluids. That will replace the constant loss of water through the urine.
 In central diabetes insipidus, the missing ADH can be replaced using the medication vasopressin (desmopressin or DDAVP). This is often taken as a nasal spray. An oral preparation is also available. There are also other therapies available that help enhance the action of ADH.
In central diabetes insipidus, the missing ADH can be replaced using the medication vasopressin (desmopressin or DDAVP). This is often taken as a nasal spray. An oral preparation is also available. There are also other therapies available that help enhance the action of ADH.
Other medicines may improve the symptoms of nephrogenic diabetes insipidus. They include indomethacin (Indocin) and, surprisingly, diuretics (hydrochlorothiazide or amiloride.
Gestational diabetes is a condition characterized by high blood sugar (glucose) levels that is first recognized during pregnancy. The condition occurs in approximately 4% of all pregnancies.
What is Gestational Diabetes?
Pregnancy and Gestational Diabetes
Diabetes can affect the developing fetus throughout the pregnancy. In early pregnancy, a mother’s diabetes can result in birth defects and an increased rate of miscarriage.
Gestational Diabetes Symptoms
Because gestational diabetes does not cause symptoms, you need to be tested for the condition.
Gestational Diabetes Causes
During pregnancy, an organ called the placenta develops in the uterus. The placenta connects the mother and baby and makes sure the baby has enough food and water. It also makes several hormones. Some of these hormones make it hard for insulin to do its job-controlling blood sugar-so the mother’s body has to make more insulin to keep sugar levels in a safe range. Gestational diabetes develops when the organ that makes insulin, the pancreas, cannot make enough insulin to keep blood sugar levels within a target range.
Are You at Risk for Gestational Diabetes?
If you have had gestational diabetes before, or if your doctor is concerned about your risk of developing gestational diabetes, a test may be performed before the 13th week of pregnancy.
Gestational Diabetes Screening and Tests
All pregnant women should be screened for gestational diabetes during their pregnancy. Screening may be done by taking the woman’s medical history, examining certain risk factors, or screening with an oral glucose tolerance test.
Treatment for Gestational Diabetes
If you have gestational diabetes, you will be asked to take certain dietary and lifestyle measures to keep your blood sugar at a safe level.
Preventing Gestational Diabetes
In some women, gestational diabetes cannot be prevented. But you may be able to lower your chance of getting gestational diabetes by staying at a healthy weight and not gaining too much weight during pregnancy
What Is Prediabetes?
People with prediabetes have glucose levels that are higher than normal but not high enough yet to indicate diabetes. The condition used to be called borderline diabetes.
Prediabetes, also known as “impaired glucose tolerance” or “impaired fasting glucose,” is a health condition with no symptoms. It is almost always present before a person develops the more serious type 2 diabetes
More and more, doctors are recognizing the importance of diagnosing prediabetes as treatment of the condition may prevent more serious health problems.
Insulin Resistance and Diabetes
Insulin resistance or metabolic syndrome describes a combination of health problems that have a common link — an increased risk of diabetes and early heart disease.
What Are the Symptoms of Prediabetes?
Although most people with prediabetes have no symptoms at all, symptoms of diabetes may include unusual thirst, a frequent need to urinate, blurred vision, or extreme fatigue.
A medical lab test may show some signs that suggest prediabetes may be present.
Who Should Be Tested for Prediabetes?
You should be tested for prediabetes if:
How Is Diabetes Insipidus Treated?
 You’re 45 years of age or older.
You’re 45 years of age or older.
 You’re overweight with a BMI (body mass index) of 25 or over and have any of the following risk factors for diabetes:
You’re overweight with a BMI (body mass index) of 25 or over and have any of the following risk factors for diabetes:
 You are physically inactive.
You are physically inactive.
 You have a first degree relative with diabetes.
You have a first degree relative with diabetes.
 You belong to a high risk ethnic group.
You belong to a high risk ethnic group.
 You have a history of gestational diabetes or delivering a baby that weighed more than 9 pounds.
You have a history of gestational diabetes or delivering a baby that weighed more than 9 pounds.
 You have polycystic ovary syndrome.
You have polycystic ovary syndrome.
 You have high triglycerides or low HDL (good) cholesterol.
You have high triglycerides or low HDL (good) cholesterol.
 You have had abnormal blood sugar tests in the past.
You have had abnormal blood sugar tests in the past.
 You have a history of heart disease.
You have a history of heart disease.
 You have any signs of a condition called insulin resistance (such as severe obesity or a skin condition called acanthosis nigricans).
You have any signs of a condition called insulin resistance (such as severe obesity or a skin condition called acanthosis nigricans).
Prediabetes: What Increases Your Risk
The risk factors for prediabetes are similar to those for type 2 diabetes. Most people who get type 2 diabetes had prediabetes first.
How Is Prediabetes Diagnosed?
To determine if you have prediabetes, your doctor can perform one of three different blood tests — the fasting plasma glucose (FPG) test, the oral glucose tolerance test (OGTT), or the hemoglobin A1C (or average blood sugar) test
Why Is It Important to Recognize and Treat Prediabetes?
By identifying the signs of prediabetes before diabetes occurs, you can prevent type 2 diabetes altogether and lower your risk of complications associated with this condition, such as heart disease.
A recently completed research study called the Diabetes Prevention Program (DPP) found that many people who made healthy changes in their diet and who increased their physical activity were able to prevent diabetes. And many were able to return their blood sugar levels back into the normal range. The DPP found that just 30 minutes of moderate physical activity a day coupled with a 7% weight loss produced almost a 60% reduction in diabetes.
What’s the Treatment for Prediabetes?
To successfully treat prediabetes:
 Eat a heart healthy diet and lose weight. A 5% to 10% weight loss can make a huge difference.
Eat a heart healthy diet and lose weight. A 5% to 10% weight loss can make a huge difference.
 Exercise – Try to work up to 30 minutes of exercise a day, 5 days a week. The activity can be split into several short periods: 3 sessions of 10 minutes. Select an activity that you enjoy such as walking. Check with your doctor before increasing your activity level.
Exercise – Try to work up to 30 minutes of exercise a day, 5 days a week. The activity can be split into several short periods: 3 sessions of 10 minutes. Select an activity that you enjoy such as walking. Check with your doctor before increasing your activity level.
 Stop smoking.
Stop smoking.
 Treat high blood pressure and high cholesterol.
Treat high blood pressure and high cholesterol.
Why is blood sugar checked at home?
Home blood sugar (glucose) testing is an important part of controlling blood sugar. One important goal of diabetes treatment is to keep the blood glucose levels near the normal range of 70 to 120 mg/dl before meals and under 140 mg/dl at two hours after eating. Blood glucose levels are usually tested before and after meals, and at bedtime.
Diet modification: The first step for the ayurvedic treatment of diabetes it is necessary to modify diet, which includes reduced intake of sugar and simple carbohydrates, and emphasizes on complex carbohydrates. Protein intake should be decreased as higher intake can damage the kidneys. Fat intake should be also limited as digestion of fat becomes difficult in these patients due to deficiency of other pancreatic enzymes. Eat plenty of fresh vegetables, orange, lemons, bitter fruits and herbs.
Panchakarma: Many diabetics have antibodies against their own pancreatic tissue (autoantibodies), hence the cleansing program Panchakarma is used to clear the auto antibodies. This includes herbal massages, herbal steam sauna, and fasting to cleanse the body. Following these a herbal purge for the liver, pancreas, and spleen is given. Lastly colon therapy is given to cleanse the digestive tract and then to reorganise the system.
Herbs: Several herbal remedies for treatment of diabetes are used by ayurveda practitioners. Shilajit, gudmar turmeric, neem, amalaki, guggul, and arjuna are the most important herbal remedies for treatment of diabetes. Turmeric along with aloe-vera gel is effective in the early stages of diabetes for regulating function of pancreas and liver.
Studies have shown that herbs such as Coccinea indica, holy basil, fenugreek, and Gymnema sylvestre have glucose-lowering effect.
Some of the commonly used Ayurvedic herbal remedies for diabetes mellitus are
1. Bitter gourd or bitter lemon juice taken everyday in empty stomach.
2. Turmeric capsules: 2 capsules daily thrice a day
3. Rose apple stones powder taken twice daily.
4. Fenugreek, musta, Arjuna, triphala, ajwan, haritaki mixed with ghee taken daily.
5. Amlaki powder, haldi powder with honey, taken twice daily.
These remedies lower the blood sugar and mostly decrease the need for insulin and other allopathic medicines to control blood sugar.
Caution with Ayurveda
Ayurvedic medicines are effective for treating diabetes but relying on this type of treatment alone can have adverse health consequences. Consult your allopathic physician before you stop the allopathic drugs for diabetes treatment. Some of the ayurvedic medicines can interact with medicines, foods, or dietary supplements. Inform your allopathic physician if you are using ayurvedic remedies.
Exercise and yoga: Physical exercise, breathing exercises and yoga are used for ayurvedic treatment for diabetes.
 |
Easy Pose (Sukhasana) This is one of the classic Meditative Poses and is usually performed after doing the Corpse Pose. The Easy Pose helps in straightening the spine, slowing down metabolism, promoting inner tranquility, and keeping your mind still. |
 |
Shoulder Stretches Shoulder Stretches are great in relieving stress and tension on your shoulders, as well as your entire upper back. Practice them daily for several weeks and notice the changes. Learn some basic stretches for the shoulders in this section. |
 |
Sun Salutation (Surya Namaskar) The Sun Salutation or Surya Namaskar is a Yoga Pose which limbers up the whole body in preparation for the Yoga Asanas. It is a graceful sequence of twelve Yoga positions performed as one continuous exercise. Learn how to practice Sun Salutation in this section. |
 |
Half Spinal Twist (Ardha Matsyendrasana) If done properly, the Half Spinal Twist lengthens and strengthens the spine. It is also beneficial for your liver, kidneys, as well as adrenal glands. Practice this Yoga Pose under the supervision of a Yoga instructor. In this section, learn how to perform the Half Spinal Twist. |
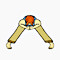 |
Stand Spread Leg Forward Fold Practicing the Standing Spread Leg Forward Fold can strengthen and stretch your inner and back legs and your spine. People with lower back problems should avoid doing the full forward bend. For beginners, you may use props like a folding chair to support your forearms. |
 |
Tree Pose (Tadasana) The Tree Pose helps strengthen your thighs, calves, ankles and back. It can also increase the flexibility of your hips and groin. Your balance and concentration can also be improved with constant practice. This Yoga Pose is recommended for people who have sciatica and flat feet. |
 |
Double Leg Raises A Double Leg Raise is similar to a Single Leg Raise, only this time, you will raise both legs. In doing this Yoga Pose, make sure that the full length of your back is resting on the floor and your shoulders and neck are relaxed. This section covers the steps and guidelines on how to do this pose properly. |
 |
Fish Pose (Matsyasana) Doing the Fish Pose relieves stiffness of the neck and shoulder muscles and improves flexibility of your spine. It is the counter-pose of the Shoulderstand. Hold the Fish Pose for at least half the amount of time you spent in the Shoulderstand in order to balance the stretch. |
 |
Yoga Exercise – Corpse Pose (Savasana) The Corpse Yoga Pose is considered as a classic relaxation Yoga Pose and is practiced before or in between Asanas as well as a Final Relaxation. While it looks deceptively simple, it is actually difficult to perform. Learn more on how to do it with the help of this article. |
 |
Kapalabhati Kapalabhati is a Breathing Technique used specifically for cleansing. If you have a lot of mucus in the air passages or feel tension and blockages in the chest it is often helpful to breathe quickly. This article will introduce you to this breathing techniques and show you its its benefits. |
 |
Simple Meditation Technique This Meditation process is good to induce relaxation response and promotes a peaceful and relaxed mind. Meditation has also been scientifically proven to have health benefits such as lowering blood pressure and aiding the asthmatics in their breathing. |
 |
Anuloma Viloma Anuloma Viloma is also called the Alternate Nostril Breathing Technique. In this Breathing Technique, you inhale through one nostril, retain the breath, and exhale through the other nostril. Learn how to do this technique for beginners by following the steps found in this article. |
 |
Relaxation Pose There are three parts to proper relaxation – physical, mental and spiritual relaxation. Relaxation Yoga Pose relaxes your body and mind, and makes you feel refreshed after doing the Asanas and the pranayama. This is why it is an essential part of Yoga practice. |