Toll Free No.: 1800 2330 0007 email: admin@dhanwantari.com

MusculoSkeletal System
The human musculoskeletal system consists of the human skeleton, made by bones attached to other bones with joints, and skeletal muscle attached to the skeleton by tendons.
Bones
An adult human has approximately 206 distinct bones:
 |
Spine and vertebral column (26) | |
 |
Cranium (8) | |
 |
Face (14) | |
 |
Hyoid bone, sternum and ribs (26) | |
 |
Upper extremities (70) | |
 |
Lower extremities (62) |
Skeletal System Overview
The Skeleton is a rigid framework that provides protection and structure in many types of animals.
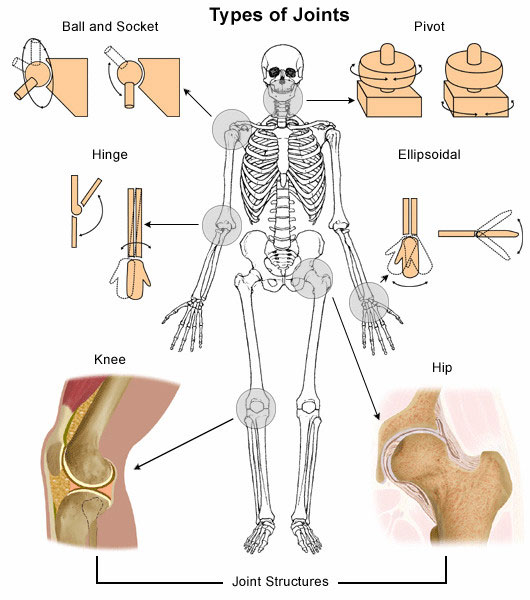
The average adult human skeleton has around 206 bones. These bones meet at joints, the majority of which are freely movable. The skeleton also contains cartilage for elasticity. Ligaments are strong strips of fibrous connective tissue that hold bones together at joints, thereby stabilizing the skeleton during movement.
The Skeletal System serves many important functions; it provides the shape and form for our bodies in addition to supporting, protecting, allowing bodily movement, producing blood for the body, and storing minerals.
Its 206 bones form a rigid framework to which the softer tissues and organs of the body are attached.
Vital organs are protected by the skeletal system. The brain is protected by the surrounding skull as the heart and lungs are encased by the sternum and rib cage.
Bodily movement is carried out by the interaction of the muscular and skeletal systems. For this reason, they are often grouped together as the musculo-skeletal system. Muscles are connected to bones by tendons. Bones are connected to each other by ligaments. Where bones meet one another is typically called a joint. Muscles which cause movement of a joint are connected to two different bones and contract to pull them together. An example would be the contraction of the biceps and a relaxation of the triceps. This produces a bend at the elbow. The contraction of the triceps and relaxation of the biceps produces the effect of straightening the arm.
Blood cells are produced by the marrow located in some bones. An average of 2.6 million red blood cells are produced each second by the bone marrow to replace those worn out and destroyed by the liver.
Bones serve as a storage area for minerals such as calcium and phosphorus. When an excess is present in the blood, buildup will occur within the bones. When the supply of these minerals within the blood is low, it will be withdrawn from the bones to replenish the supply.
The human skeleton is divided into two distinct parts:
The axial skeleton consists of bones that form the axis of the body and support and protect the organs of the head, neck, and trunk.
 |
The Skull | |
 |
The Sternum | |
 |
The Ribs | |
 |
The Vertebral Column |
The appendicular skeleton is composed of bones that anchor the appendages to the axial skeleton.
 |
The Upper Extremities | |
 |
The Lower Extremities | |
 |
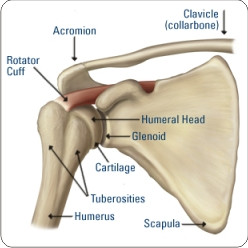
The Shoulder Girdle |
|
 |
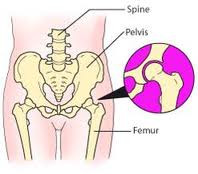
The Pelvic Girdle--(the sacrum and coccyx are considered part of the vertebral column) |
MUSCULOSKELETAL SYSTEM PHYSIOLOGY
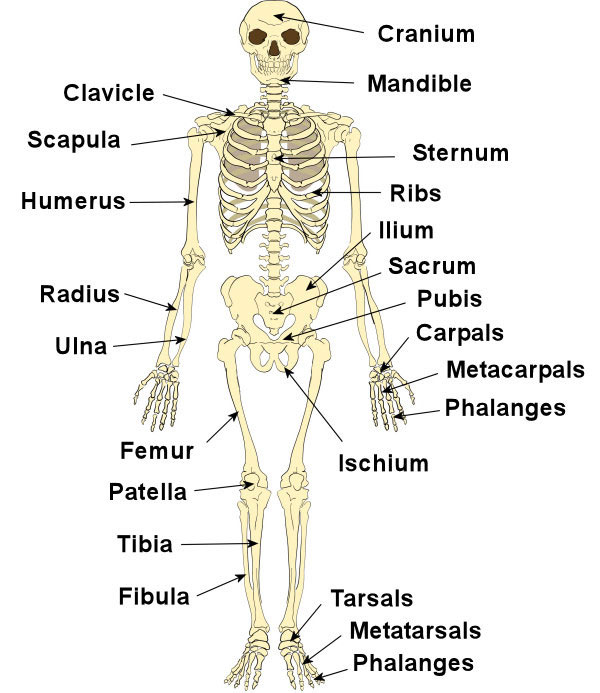
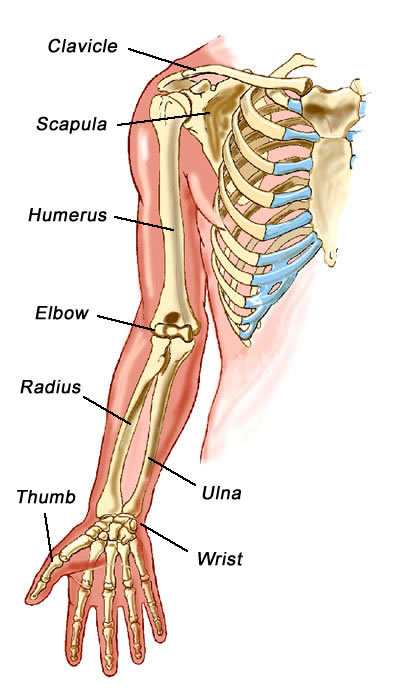
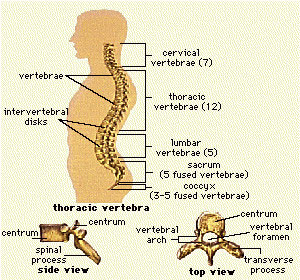
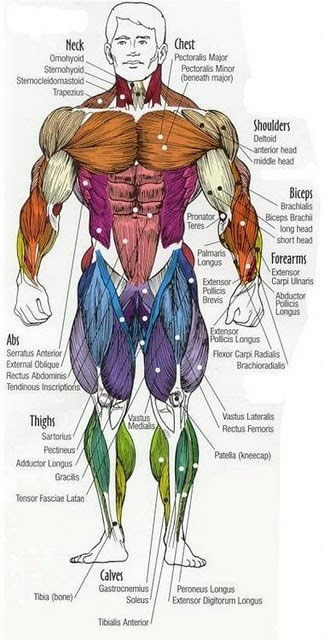
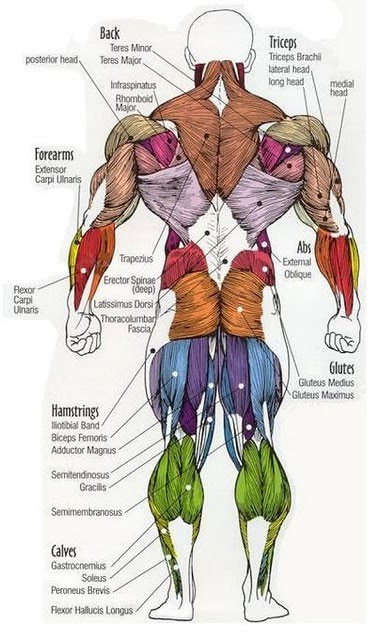
The musculoskeletal system consists of bones, joints, ligaments, muscles, and tendons. The skeleton gives shape to the body, provides physical support and protection for the organs, stores minerals, is responsible for blood cell formation, and provides sites for muscle attachment. The action of muscles holds the skeleton upright and creates physical movement of the body. First figure depicts the bones of the skeleton. Next figures illustrate the major muscles of the body. Any disease or disorder of this system greatly affects activities of daily living.
The skeletal system consists of bones formed from osseous tissue that provide structure and function to the overall body. Also included in the skeletal system is the cartilage that forms the joints between bones and the ligaments that hold bones together at the joints. Bones can be subdivided into long bones (arms, legs, hands, and feet), short bones (wrist, ankles, and knee caps), flat bones (ribs, sternum, shoulder blades, hip bones, and cranial bones), and irregular bones (vertebrae and facial bones).
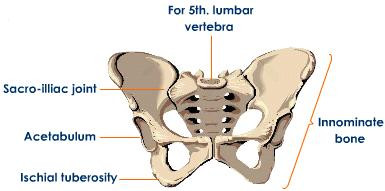
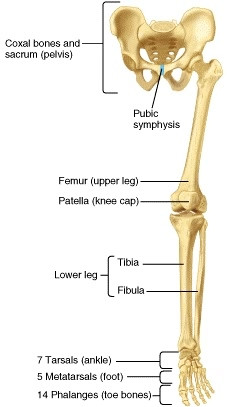
The adult skeletal system has two divisions: the axial skeletal system and the appendicular skeletal system. The axial skeleton is the center portion of the body and includes the bones of the skull, hyoid bone, bones of the middle ear, vertebral column, and rib cage. The appendicular skeleton is composed of the bones of the appendages or limbs and includes the bones of the arms and legs, the shoulders, and the pelvic girdle.
There are two types of bone: compact and spongy. Compact bone is the dense, hard tissue found in the shafts of long bones. Yellow marrow, which is composed of fat, is stored in these bones. Spongy bone, or cancellous bone, is less dense and is found at the ends of long bones and in the other bones of the body.
The muscular system holds the body upright and moves the skeletal system. Muscles have specialized cells for contraction wherein they shorten and pull a bone to produce movement. Muscle movement creates heat that helps to regulate body temperature.
There are three types of muscles:
| 1. | Skeletal muscle is also called voluntary muscle because it is attached to the skeleton and its movement is consciously controlled. The cells of this type of muscle are elongated and have the ability to stretch and return to their previous shape. | |
| 2. | Smooth muscle is also called involuntary or visceral muscle because it is found in the walls of organs and its function is not consciously controlled. This type of muscle has shorter cells with tapered ends and cannot stretch as much as skeletal muscle. | |
| 3. | Cardiac muscle is found only in the heart. This muscle is a combination of skeletal and smooth muscle. It is involuntarily controlled but has the ability to contract. |
 |
 |
 |
 |
 |
 |
Types of Bones
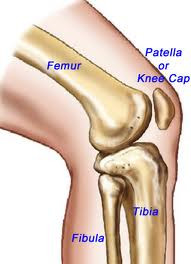
The bones of the body fall into four general categories: long bones, short bones, flat bones, and irregular bones. Long bones are longer than they are wide and work as levers. The bones of the upper and lower extremities (ex. humerus, tibia, femur, ulna, metacarpals, etc.) are of this type. Short bones are short, cube-shaped, and found in the wrists and ankles. Flat bones have broad surfaces for protection of organs and attachment of muscles (ex. ribs, cranial bones, bones of shoulder girdle). Irregular bones are all others that do not fall into the previous categories. They have varied shapes, sizes, and surfaces features and include the bones of the vertebrae and a few in the skull.
Bone Composition
Bones are composed of tissue that may take one of two forms. Compact, or dense bone, and spongy, or cancellous, bone. Most bones contain both types. Compact bone is dense, hard, and forms the protective exterior portion of all bones. Spongy bone is inside the compact bone and is very porous (full of tiny holes). Spongy bone occurs in most bones. The bone tissue is composed of several types of bone cells embedded in a web of inorganic salts (mostly calcium and phosphorus) to give the bone strength, and collagenous fibers and ground substance to give the bone flexibility.
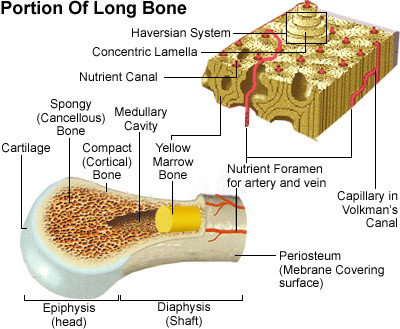
A living bone consists of three layers: the periosteum, or outside skin of the bone; the hard compact bone; and the bone marrow.
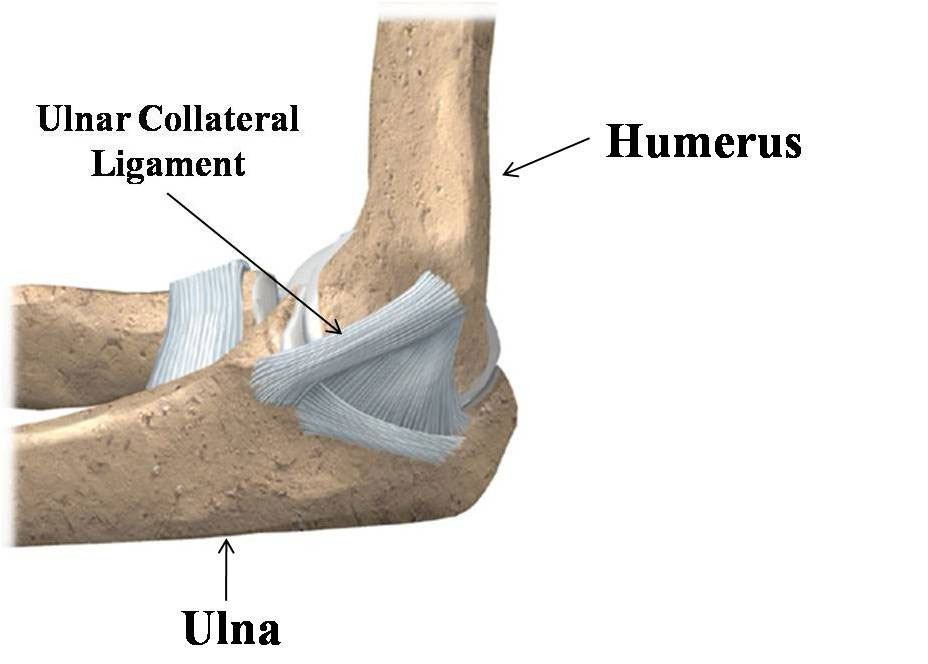
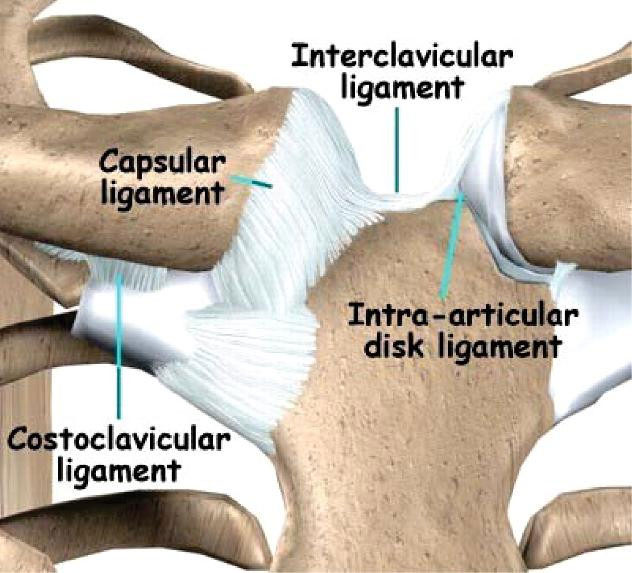
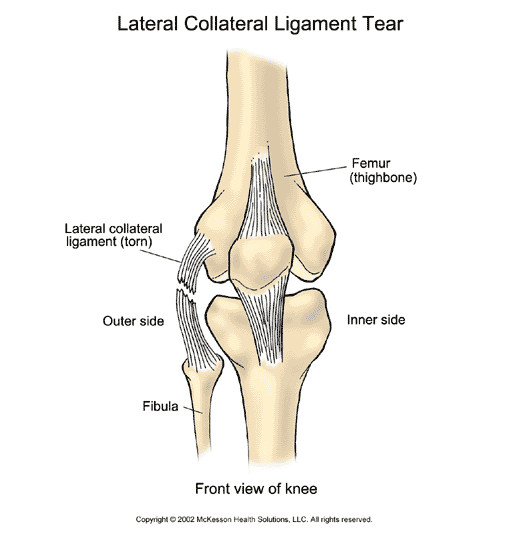
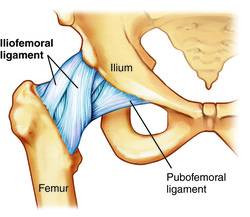
Ligaments
A ligament is a tough band of white, fibrous, slightly elastic tissue.
This is an essential part of the skeletal joints; binding the bone ends together to prevent dislocation and excessive movement that might cause breakage. Ligaments also support many internal organs; including the uterus, the bladder, the liver, and the diaphragm and helps in shaping and supporting the breasts. Ligaments, especially those in the ankle joint and knee, are sometimes damaged by injury. A "torn" ligament usually results from twisting stress when the knee is turned while weight is on that particular leg. Minor sprains are treated with ice, bandages and sometimes physical therapy, but if the ligament is torn, the joint may be placed in a plaster cast to allow time to heal or it may require surgical repairs.
If a ligament is made up of several thick bands of fibrous branches, it is called a "collateral ligament."
The word "ligament" comes from the Latin word, "ligamentum," meaning a band or tie.
 |
 |
 |
 |
 |
 |
 |
 |
 |
 |
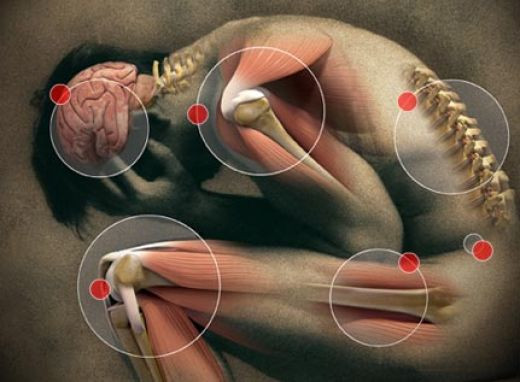
Muscle pain
Myofascial pain syndrome (MPS) is a fancy way to describe muscle pain. It refers to pain and inflammation in the body's soft tissues.
Myofascial pain is a chronic condition that affects the fascia (connective tissue that covers the muscles). Myofascial pain syndrome may involve either a single muscle or a muscle group. In some cases, the area where a person experiences the pain may not be where the myofascial pain generator is located. Experts believe that the actual site of the injury or the strain prompts the development of a trigger point that, in turn, causes pain in other areas. This situation is known as referred pain.
What Causes Myofascial Pain?
 |
Injury to muscle fibers | |
 |
Repetitive motions | |
 |
Lack of activity (such as having a broken arm in a sling) |
What Are the Symptoms of Myofascial Pain?
Myofascial pain symptoms usually involve muscle pain with specific "trigger" or "tender" points. The pain can be made worse with activity or stress. In addition to the local or regional pain associated with myofascial pain syndrome, people with the disorder also can suffer from depression, fatigue and behavioral disturbances.
How Is Myofascial Pain Diagnosed?
Trigger points can be identified by pain that results when pressure is applied to an area of a person's body. In the diagnosis of myofascial pain syndrome, two types of trigger points can be distinguished:
 |
An active trigger point is an area of extreme tenderness that usually lies within the skeletal muscle and which is associated with a local or regional pain. | |
 |
A latent trigger point is a dormant (inactive) area that has the potential to act like a trigger point. It may cause muscle weakness or restriction of movement. |
How Is Myofascial Pain Treated?
Medications such as non-steroidal anti-inflammatories, acetaminophen or opioids may be used to treat myofascial pain. Medications for sleep, depression or muscle spasm are sometimes used, as well. Non-drug treatments may include:
 |
Physical therapy | |
 |
"Stretch and spray" technique: This treatment involves spraying the muscle and trigger point with a coolant and then slowly stretching the muscle. | |
 |
Massage therapy | |
 |
Trigger point injection |
In some chronic cases of myofascial pain, combinations of physical therapy, trigger point injections, and massage are needed.
Muscular Dystrophy
Dystrophy is any condition in which a part of the body weakens or wastes away. In muscular dystrophy, the weakness is in the muscles. An inherited genetic mistake prevents the body from making a protein that helps build muscles and keep them strong.
Children who are born with muscular dystrophy usually develop normally for the first few years of life. They may suddenly show signs of clumsiness. These signs include:
 |
trouble walking | |
 |
difficulty raising the front of their foot (called foot drop) | |
 |
falling |
Over time, children with muscular dystrophy can become weaker and weaker, losing the ability to sit, walk, and lift objects. Because the disease can also affect muscles in the heart and lungs, serious heart and breathing problems can occur.
There are several different types of muscular dystrophy. Muscle weakness is a hallmark of each type. But the symptoms can vary and start at different ages.
Some muscular dystrophies are mild. Others are severe and cause greater muscle loss.
Duchenne Muscular Dystrophy
Duchenne muscular dystrophy is the most common and severe form of the disease. It usually starts when a child is between ages 2 and 5.
Symptoms of Duchenne muscular dystrophy include:
 |
Muscle weakness that begins in the hips, pelvis, and legs | |
 |
Difficulty standing | |
 |
Trouble learning to sit independently and walk | |
 |
Unsteady, waddling gait | |
 |
Walking on the toes or balls of the feet | |
 |
Clumsiness, falling often | |
 |
Trouble climbing stairs | |
 |
Difficulty rising from a lying or sitting position | |
 |
Larger-than-normal calves that are sometimes painful | |
 |
Trouble breathing | |
 |
Learning disabilities or behavioral problems | |
 |
Curvature of the spine (scoliosis). This can cause one hip to rise higher than the other. | |
 |
Breathing problems that may eventually require the use of a ventilator |
By age 12, most children with Duchenne muscular dystrophy must use a wheelchair to get around. The disease also damages the heart and the muscles needed to breathe, which can be life threatening.
Becker Muscular Dystrophy
The symptoms of Becker muscular dystrophy are similar to those of Duchenne muscular dystrophy. But Becker muscular dystrophy starts later -- around the teen years. It also develops much more slowly.
The first signs of Becker muscular dystrophy may be trouble walking fast, running, and climbing stairs. Other symptoms may include:
 |
Muscle weakness that starts in the pelvis, shoulders, hips, and thighs | |
 |
Difficulty learning how to walk | |
 |
Waddling gait | |
 |
Walking on the toes | |
 |
Larger-than-normal calves | |
 |
Muscle cramps when exercising | |
 |
Trouble lifting objects above waist height because of shoulder and arm weakness | |
 |
Heart and breathing problems (later in life) |
Often children with Becker muscular dystrophy can walk. As they get older they may need to use a cane or wheelchair to get around.
Myotonic Dystrophy
The symptoms of myotonic dystrophy may be obvious from birth or they can develop later -- during the teenage or adult years.
Like other forms of muscular dystrophy, myotonic dystrophy leads to muscle weakness that gets worse over time. But it usually affects small muscles, like those in the:
 |
face | |
 |
neck | |
 |
hands |
Symptoms of myotonic dystrophy can start at any time in a person's life. The symptoms include:
 |
Weakness in the muscles of the face, arms, hands, and neck | |
 |
Muscle stiffness (myotonia) -- difficulty relaxing the muscles after they are tightened | |
 |
Shrinking of the muscles over time (muscle wasting) | |
 |
Cataracts -- clouding of the eye's lens | |
 |
Daytime sleepiness | |
 |
Learning and behavioral problems | |
 |
Heart problems, including irregular heartbeat (arrhythmia) |
The type of myotonic dystrophy that begins at birth is more severe. Other forms get worse very slowly, and can take 50 or 60 years to progress.
Limb-Girdle Muscular Dystrophy
This form of muscular dystrophy is actually a group of related conditions. It usually starts in childhood or during the teenage years.
Often the muscles that become weak first are the big muscles of the:
 |
pelvis | |
 |
shoulders | |
 |
hips |
The muscle weakness gets worse very slowly over time.
Other symptoms include:
 |
Loss of muscle in affected areas | |
 |
Back pain | |
 |
Trouble lifting objects | |
 |
Difficulty running | |
 |
Fast heartbeat (palpitations) or irregular heartbeat |
How serious the effects are depends on the child. Some children have only mild muscle weakness. Others are so weak they need to use a wheelchair.
In its later stages, limb-girdle muscular dystrophy can cause serious heart problems.
Facioscapulohumeral Muscular Dystrophy
Usually this type of muscular dystrophy doesn't appear until the teenage years or later in life. It also gets worse very slowly. Some people may not realize they have it until they are already old.
Symptoms include:
a
 |
Muscle weakness in the face. This affects the child's ability to close the eyes and purse the lips (whistle). | |
 |
Muscle weakness in the shoulders, upper arms, upper back, and lower legs | |
 |
Difficulty raising the arms or lifting objects because of muscle weakness in the shoulders and back |
One side of the body may be more severely affected than the other.
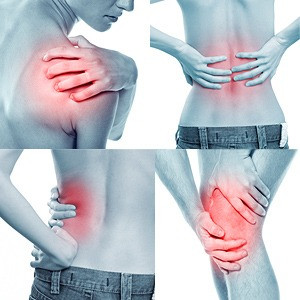
ARTHRITIS
Arthritis is a general term that means inflammation of the joints.
 |
 |
What Are the Common Types of Arthritis?
There are two major types of arthritis -- osteoarthritis, which is the "wear and tear" arthritis, and rheumatoid arthritis, an inflammatory type of arthritis that happens when the body's immune system does not work properly.
Gout, which is caused by crystals that collect in the joints, is another common type of arthritis. Psoriatic arthritis, lupus, and septic arthritis are other types of the condition.
Joint pain and progressive stiffness without noticeable swelling, chills, or fever during normal activities probably indicates the gradual onset of osteoarthritis.
Painful swelling, inflammation, and stiffness in the fingers, arms, legs, and wrists occurring in the same joints on both sides of the body, especially upon awakening, may be signs of rheumatoid arthritis.
Fever, joint inflammation, tenderness, and sharp pain, sometimes accompanied by chills and associated with an injury or another illness, may indicate infectious arthritis.
In children, intermittent fever, loss of appetite, weight loss, and anemia, or blotchy rash on the arms and legs, may signal the onset of some types of juvenile rheumatoid arthritis. Other forms of juvenile rheumatoid arthritis are associated with joint stiffness, a limp, or joint swelling.
 |
 |
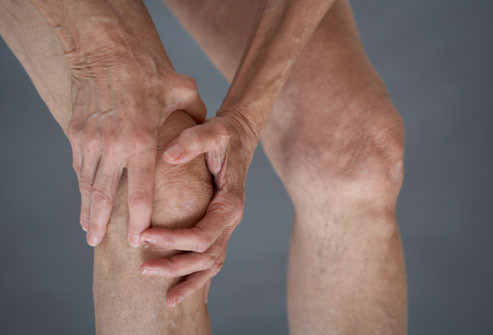
Osteoarthritis
Osteoarthritis, commonly known as wear and tear arthritis, is the most common type of arthritis. It is associated with a breakdown of cartilage in joints and can occur in almost any joint in the body. It commonly occurs in the weight bearing joints of the hips, knees, and spine. It also affects the fingers, thumb, neck, and large toe. Osteoarthritis -- also called OA -- usually does not affect other joints unless previous injury or excessive stress is involved.
Cartilage is a firm, rubbery material that covers the ends of bones in normal joints. Its main function is to reduce friction in the joints and serve as a "shock absorber." The shock-absorbing quality of normal cartilage comes from its ability to change shape when compressed (flattened or pressed together).
Osteoarthritis causes the cartilage in a joint to become stiff and lose its elasticity, making it more susceptible to damage. Over time, the cartilage may wear away in some areas, greatly decreasing its ability to act as a shock absorber. As the cartilage deteriorates, tendons and ligaments stretch, causing pain. If the condition worsens, the bones could rub against each other.
The chance of developing the disease increases with age. Most people over age 60 have osteoarthritis to some degree, but its severity varies. Even people in their 20s and 30s can get osteoarthritis. In people over 50, more women than men have osteoarthritis.
Hip problems
Hip problems may develop from overuse, bone changes with age, tumors, infection, changes in the blood supply, or a problem that was present from birth (congenital).
Pain when resting
Pain with movement
Pain with weight-bearing
Knee Osteoarthritis
Osteoarthritis in the knee begins with the gradual deterioration of cartilage. Without the protective cartilage, the bones begin to rub together, causing pain, loss of mobility, and deformity
Hand Osteoarthritis
In the joint located at the base of the thumb, where the thumb meets the wrist. You may have bumps or bony knobs located near the site of the arthritis.
In the joint at the end of the finger closest to the nail
In the joint in the middle of the finger
How Is Osteoarthritis Treated?
 |
Osteoarthritis usually is treated by a combination of treatments, including exercise, weight loss if needed, medications, physical therapy with muscle strengthening exercises, hot and cold compresses to the painful joint, removal of joint fluid, injection of medications into the joint, and use of supportive devices such as crutches or canes. Surgery may be helpful to relieve pain when other treatment options have not been effective. | |
 |
The type of treatment will depend on several factors including your age, activities and occupation, overall health, medical history, location of your osteoarthritis, and severity of the condition. |
How Does Weight and Exercise Impact Osteoarthritis?
 |
Staying at your recommended weight helps prevent osteoarthritis of the knees, hips, and spine, reduces the stress on these weight-bearing joints, and reduces pain in joints already affected. Once you have osteoarthritis, losing weight also can relieve the stress and pain in your knees. | |
 |
Exercise is important to improve joint movement and to strengthen the muscles that surround the joints. Gentle exercises, such as swimming or walking on flat surfaces, are recommended because they are less stressful on your joints. Avoid activities that increase joint pain, such as jogging or high impact aerobics. Exercises that strengthen the muscles reduce pain in patients with osteoarthritis, particularly with osteoarthritis of the knee. |
What Medications Are Used to Treat Osteoarthritis?
 |
The first step with medication is often over-the-counter pain relievers as needed. These include acetaminophen (Tylenol), ibuprofen (Advil, Motrin), and naproxen (Aleve). Don't take over-the-counter medications for more than 10 days without checking with your doctor. Taking them longer than that increases the chance of side effects | |
 |
Some medications in the form of creams, rubs, or sprays may be applied over the skin of affected areas to relieve pain. For some people with persistent pain despite these pills or creams, steroids can be injected directly into the joint. These injections can be given several times a year, though some experts believe this may ultimately accelerate joint damage. | |
 |
Some medications in the form of creams, rubs, or sprays may be applied over the skin of affected areas to relieve pain. For some people with persistent pain despite these pills or creams, steroids can be injected directly into the joint. These injections can be given several times a year, though some experts believe this may ultimately accelerate joint damage. | |
 |
When osteoarthritis pain is severe and other treatments are not working, some doctors will give stronger pain pills, such as narcotics. | |
 |
Unfortunately, none of these will reverse or slow the progression of joint damage caused by osteoarthritis. |
Acupuncture has also been shown to provide significant and immediate pain relief in some people with osteoarthritis.
There are several types of surgery for osteoarthritis
Arthroscopy to clean out the damaged cartilage or repair tissues
Joint replacement surgery to replace the damaged joint with an artificial one.
Joint fusion to remove the damaged joint and fuse the two bones on each side of the joint.
Rheumatoid Arthritis
The most serious side effect that can occur after influenza vaccination is an allergic reaction in people who have a severe allergy to eggs. For this reason, people who have an allergy to eggs should not receive the influenza vaccine.
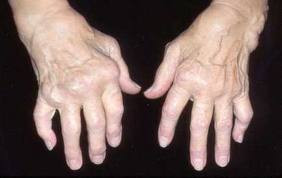
Rheumatoid arthritis is a type of chronic arthritis that typically occurs in joints on both sides of the body (such as hands, wrists, or knees). This symmetry helps distinguish rheumatoid arthritis from other types of arthritis.
In addition to affecting the joints, rheumatoid arthritis may occasionally affect the skin, eyes, lungs, heart, blood, or nerves.
What Are the Symptoms of Rheumatoid Arthritis?
Symptoms of rheumatoid arthritis include:

| Joint pain and swelling | |

| Stiffness, especially in the morning or after sitting for long periods | |

| Fatigue |
Rheumatoid arthritis affects everyone differently. For some, joint symptoms develop gradually over several years. In others, rheumatoid arthritis may progress rapidly, while other people may have rheumatoid arthritis for a limited period of time and then enter a period of remission
What Causes Rheumatoid Arthritis?
The exact cause of rheumatoid arthritis is unknown, but it is thought to be due to a combination of genetic, environmental, and hormonal factors. With rheumatoid arthritis, something seems to trigger the immune system to attack the joints and sometimes other organs
How Is Rheumatoid Arthritis Treated?
There are many different ways to treat rheumatoid arthritis. Treatments include medications, rest and exercise, and surgery to correct damage to the joint.
The type of treatment will depend on several factors, including the person's age, overall health, medical history, and severity of the arthritis
Drugs that offer relief of arthritis symptoms (joint pain, stiffness, and swelling) include:

| Anti-inflammatory painkiller drugs, such as aspirin, ibuprofen, or naproxen | |

| Topical (applied directly to the skin) pain relievers | |

| Corticosteroids, such as prednisone | |

| Narcotic pain relievers |
A balance of rest and exercise is important in treating rheumatoid arthritis
When joint damage from the rheumatoid arthritis has become severe or pain is not controlled with drugs, surgery may be an option to help restore function to a damaged joint
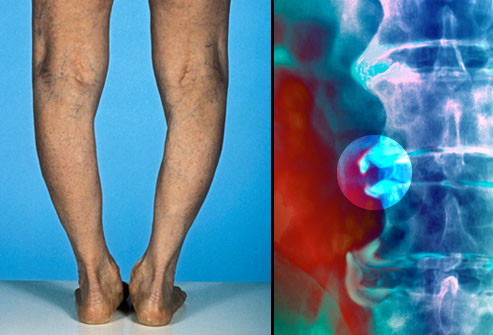
Degenerative Disc Disease
Degenerative disc disease is not really a disease but a term used to describe the normal changes in your spinal discs as you age. Spinal discs are soft, compressible discs that separate the interlocking bones (vertebrae) that make up the spine. The discs act as shock absorbers for the spine, allowing it to flex, bend, and twist. Degenerative disc disease can take place throughout the spine, but it most often occurs in the discs in the lower back (lumbar region) and the neck (cervical region).
 |
 |
How is it treated?
To relieve pain, put ice or heat (whichever feels better) on the affected area and use acetaminophen (such as Tylenol) or nonsteroidal anti-inflammatory drugs, including aspirin (such as Bayer), ibuprofen (such as Advil), or naproxen (such as Aleve). Do not give aspirin to anyone younger than 20 because of the risk of Reye syndrome. Acetaminophen (such as Tylenol) also can help relieve pain. Your doctor can prescribe stronger medicines if needed.
Further treatment depends on whether the damaged disc has resulted in other conditions, such as osteoarthritis, a herniated disc, or spinal stenosis. Physical therapy and exercises for strengthening and stretching the back are often recommended, and in some cases surgery may be recommended.
Gout
Gout is a kind of arthritis. It can cause an attack of sudden burning pain, stiffness, and swelling in a joint, usually a big toe. These attacks can happen over and over unless gout is treated. Over time, they can harm your joints, tendons, and other tissues. Gout is most common in men.
Gout is caused by too much uric acid in the blood.
How is it treated?
To ease the pain during a gout attack, rest the joint that hurts. Taking ibuprofen or another anti-inflammatory medicine can also help you feel better. But don't take aspirin. It can make gout worse by raising the uric acid level in the blood.
Paying attention to what you eat may help you manage your gout. Eat moderate amounts of a healthy mix of foods to control your weight and get the nutrients you need. Avoid regular daily intake of meat, seafood, and alcohol (especially beer). Drink plenty of water and other fluids.
Psoriatic Arthritis
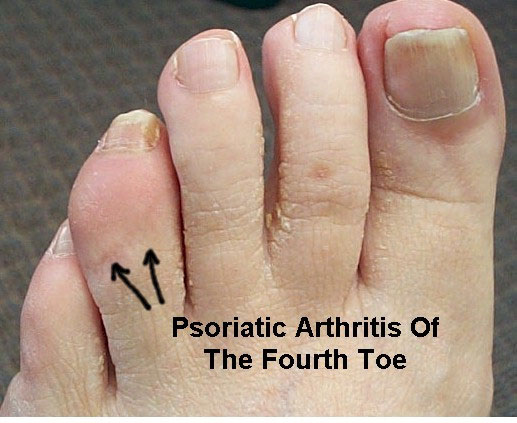
Psoriatic arthritis is a form of inflammatory arthritis. Psoriasis is a skin disease that causes a red, scaly rash most commonly over the elbows, knees, ankles, feet, hands, and other areas.
How is psoriatic arthritis treated?
Treatment for psoriatic arthritis consists of twice daily moist heat applications, exercises, and nonsteroidal anti-inflammatory drugs (NSAIDs).
Is there a cure for psoriatic arthritis?
There is no cure for psoriatic arthritis. But use of biologic agents have made remission a real possibility and goal of treatment.
AYURVEDA

Disease Process in Arthritis
According to Ayurveda mostly pains are caused by the aggravation of vata (air) dosha. Arthritis is a condition which is caused by accumulation of ama and aggravation of vata. (Ama is a toxic by-product of improper digestion.) This ama circulates in the whole body and deposits or gets collected at the sites which are weaker. When it deposits in the joints and at the same time there is aggravation of vata, it results in a disease called amavata. This amavata is arthritis.
Remedies
As described above ama and vata are the main causes, so efforts should be made to digest ama and to reduce the vata. The digestion should be improved so that no further ama is produced. Efforts should be made to relieve the pain and inflammation. This is the line of treatment according to Ayurveda.
Fasting is very beneficial for digesting the ama. The fasting be complete or partial depending on the strength of the person, season and place. Two tea spoons of lemon juice mixed in 250 ml. of warm water and a tea spoon of honey is good to take twice a day -morning and evening.
Liberal intake of orange juice or sweet limejuice or Vitamin C enhances the efficacy of any anti rheumatic drug, since Vitamin C can reduce skeletal pain.
Triphala Guggul: Improves digestive disorders & prevents toxins to reach the joints. Helps transport of beneficial drugs to the joints
Sinhanad Guggul & Yograj Guggul: Effective against inflammation,oedema of joints & joint pains.
Guggul is a very helpful herb for curing arthritis. If available it can be taken in one to 3 gm dose twice a day after meals with warm water.
Guggul preperations are available in capsule forms like ArthoRich.

Diet modification: Anti-vata diet should be taken. Avoid hot and spicy food, and other foodstuffs like dairy foods, potato, eggplant cabbage, cauliflower, broccoli, okra, potatoes etc. Consume plenty of fruits, fruit Juices, homemade soups, green salads and green vegetables.
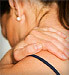
Massage: Hot baths, compresses or massage with massage oils such as Almond oil, Sesame oil is beneficial in arthritic pain as it reduces vata. Massage vigrously on the most severely affected areas for full benefits.
Body massage with sesame or mustard oil helps to reduce the vata and thus reduce the pain. The joints affected by pain can be massaged for longer time.
Physical exercise and yoga:
Exercise in moderation daily, too much exercise can cause further aggravation to your arthritic condition.
Light exercise is useful but you must know your limits: as a general rule if any exercise, including walking, causes pain after one hour, you have crossed your limit.
USEFUL PRACTICES
Asanas
 |
Tadagasana | |
 |
Shavasana and slow practice of all basic movements | |
 |
Ardha Chakrasana 1, Ardha Chakrasana 2 | |
 |
Anantasana 1, Anantasana 2 | |
 |
Vajrasana series from Yoga Sopan book | |
 |
Shavasana (when needed) | |
 |
Pavanmuktasana | |
 |
Preparatory Movements |
Cleansing Practices
 |
Agnisar 100 strokes total in 3 to 4 rounds | |
 |
Uddiyan Bandh 5 rounds (each round 30 seconds) | |
 |
Kapalbhati 5 rounds (120 strokes per round) | |
 |
Vaman Dhouti (once a week ) | |
 |
Laghoo Shankhaprakashlana (once a week ) |
Pranayama
 |
Anulom Vilom Deep Breathing (15 minutes) | |
 |
Purak with Right Nostrill followed by Bhramari Rechak (21rounds) | |
 |
Suryabhedan Pranayama with Kumbhak for 10 minutes | |
 |
Bhastrika Pranayama with Kumbhak for 10 minutes |
Cleasing Practices
Neti
Caution with Ayurveda: Ayurvedic treatment for arthritis can help to ease your very painful condition but all of the above methods should be done in moderation that suits your needs and health.
Naturotherapy
 |
 |
Mud Therapy for arthritis
Cervical Spondylosis
This is the condition where the bones of the neck (Cervical vertebrae) undergo changes of wear and tear.
Treatment
 |
Avoidance of constant bending forward and pressure over the neck. | |
 |
Gentle massage to neck, spine and shoulder followed by hot and cold affusions or neutral affusion. | |
 |
Hot and cold fomentations in case of acute spasm and pain. | |
 |
Arm contrast baths to relieve radiating pain to hands. | |
 |
Regular head and neck exercises. | |
 |
Maintenance of correct posture during all activities. |
Osteoarthritis of the Knee and Ankle Joints
Treatment
The frequency and the duration of the treatment varies depending on the severity and the effect sought.
The following treatments are useful in relieving pain and swelling of the knee and ankle joints.
 |
Gentle massage to the joints to strengthen muscles around the joints. | |
 |
Hot and cold fomentation and affusion to the joint to relieve pain and spasm. | |
 |
Cold compress to joints to treat localized inflammation and pain. | |
 |
A heating compress (pack) is also helpful in relieving pain/stiffness/swelling. | |
 |
Neutral immersion and neutral half–bath with epsom salt for 15–20 minutes. | |
 |
Contrast foot baths are also very helpful in relieving pain and spasm. | |
 |
Neutral jet, whirlpool and underwater massages help in relaxing the muscles of joints and also give relief from pain and spasm. | |
 |
Direct hot mud applications relieve pain. | |
 |
Regular exercises such as flexion and extension of the joints help to strengthen the muscles. | |
 |
It is also important to reduce the weight by following a controlled diet program |
Low Back Pain
Treatment
 |
RICE principle is to be adopted in case of acute or severe low back pain for first 24–48 hours. R – Resting the painful area. I – Ice–cold packs at repeated intervals. C – Cold compresses application frequently. E – Elevation of the affected area to help movement of accumulated blood to other areas. |
|
 |
Gentle low back massage followed by hot and cold affusions or fomentation. | |
 |
Infrared treatment to the affected area followed by direct mud application or a cold compress. | |
 |
Neutral spinal bath to relieve referred pain and numbness in the lower limbs. | |
 |
Neutral immersion and half bath with epsom salt for 10–20 minutes. | |
 |
Hot tip bath for 10–12 minutes for relieving back pain. | |
 |
Neutral jet massage, whirlpool baths and underwater massage to relax the stiff back muscles. | |
 |
Steam bath is also useful in providing muscular relaxation by its thermic effect. | |
 |
Regular back bending exercises coupled with maintenance of proper back posture, avoidance of lifting heavy weights and sudden jerks. | |
 |
Regular practice of breathing exercises help in movement of spinal cord resulting in relief from referred pains due to the compression on the nerve endings. |
Magnet Therapy
Static magnet therapy is believed to relieve pain by increasing circulation.
 |
 |
Strange Remedies for Arthritis
Potato Juice

Raw potato extract is one of the effective home remedies for arthritis. It is considered to be one of the most victorious treatments for rheumatic and arthritic problems.To prepare potato juice, you need to cut the unpeeled potatoes into thin slices.
 |
Put these slices in a big glass filled with cold water. | |
 |
Next morning, drink this water on an empty stomach. |
Copper

Copper is believed to bring relief to arthritis. Some people wear copper bracelet or ring while the others prefer to drink water kept in a copper vessel. Some people think that copper has antioxidant effects that can reduce inflammation though there is no evidence in this support, but wearing copper bracelet will not harm you any way.
When water is kept overnight in a copper container, it accumulates traces of copper. These copper traces are good for muscular system.
Bee Stings

Bee stings can keep arthritis at bay. This is a common belief of beekeepers who are exposed to frequent bee-stings during their work hours. There are a few research evidence that show that bee-stings reduce inflammation and finally, the pain.
Snake Venom
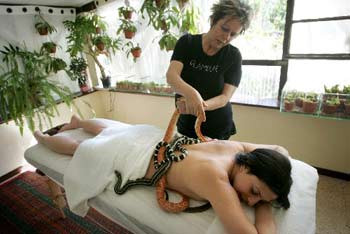
Snake venom is considered to be a strange yet effective remedy for arthritis pain. It works in the same manner as bee-sting .i.e. by reducing inflammation; but this does not mean that you chase poisonous snakes to cure arthritis. There are some proposed products that will be soon available in the market that claim to give the same effect.
Raisins Soaked in Gin

Gin-soaked raisin can cure arthritis pain. Raisins and gin have anti-inflammatory compounds that contribute to the treatment of arthritis. Until now, there has been no research done to find out the idle dose for arthritis cure, but having it for a week does produce positive results.
Cider Vinegar and Honey

Honey and cider vinegar is used to boost immune system and fight against cold. Most of us are not aware that honey and cider vinegar can also be beneficial in the treatment of arthritis pain; however, there is little scientific explanation, but evidences for its side effects are even lesser. You just need to mix equal parts of cider vinegar and honey in a glass of water and drink it everyday.
Our Recommended Products